1.Introduction
Theoretical education and clinical practice is essential to prepare students for their future professional role.[1] Clinical practice is crucial to help students learn and translate their theoretical knowledge into practical skills.[2, 3] There are different perspectives regarding the role of preceptor in traditional preceptorship and in the more recent Peer Learning (PL) supervision model. In traditional preceptorship, the preceptor’s role is to provide knowledge.[4] With PL, the preceptor has a more supportive role,[5] creating opportunities for students to become more responsible for their learning process. The preceptor’s role is to encourage the students to find the information themselves rather than giving it to the students directly.[4] In PL, the students are paired during the clinical practice period and PL is recommended as a complement to other supervision models.[5]
1.1Background
PL is a pedagogical model through which students can share experiences and knowledge as well as reflect together. This contributes to a sense of collaboration and provides the students with tools to help them solve problems together.[6] PL can offer several advantages due to all students facing the same challenges. They talk to each other in conversational language and are more open to asking questions, which can lead to a higher level of knowledge.[7] Research on PL has shown that when working together in pairs, the students can use each other for support and to mirror and reflect on mutual insecurities.[5, 8] It was reported in a qualitative study that PL enabled students to work more independently and increased their capacity to make their own critical judgements as well as solve problems together.[9] With PL the students can understand the importance of collaboration, which is a fundamental component of healthcare.[10]
According to an evaluation study by Stenberg and Carlsson,[8] PL can also lead to frustration amongst students if they start to compete for the preceptor’s attention. As a solution to this problem, Stenberg and Carlsson[8] suggest that before their clinical placement, students should be theoretically introduced to the theory of PL, including structured activities.
An increased shortage of radiographers in Sweden is predicted due to the forecast of a 15% increase in demand until 2035.[11] In Sweden, radiography is a three-year university programme (180 credits), including theoretical education and clinical practice. In the third year, students from the university in the south of Sweden undergo clinical practice in magnetic resonance imaging (MRI) at nine different hospitals.[12] Previously, there were approximately 220 new students in radiography each year in Sweden, with 160 graduating. However, in 2020 there was an enrolment increase of 27% compared to 2019.[11] Despite the lack of research on PL in the context of radiography students, there are many studies supporting PL for nursing students in clinical settings.
1.2Aim
The aim was to describe the strengths and challenges associated with a Peer Learning model in an MRI setting from preceptors' and undergraduate radiography students' perspectives.
2.Methods
2.1Design
A qualitative study design with an inductive approach. Qualitative studies provide the basis for in-depth understanding of a phenomenon.[13]
2.2Context
In this study the term preceptor refers to registered radiographers responsible for undergraduate radiographer students during their clinical practice. Students in the third year of the Bachelor radiography programme at a university in southern Sweden attend four weeks of MRI clinical practice. The goal of clinical practice in the curriculum is the ability to perform at least two MRI examinations, MRI safety and patient care in an MRI environment. The MRI environment can pose risks for staff, patients and visitors. The risks can be categorized into biological effects, burns and hearing damage, projectile effects as well as incompatibility of implantable medical devices and peripheral equipment.[14]
2.3Participants
In 2022 third year students were invited to participate in the study. The inclusion criteria were students in their final year of education who had had or were going to have a clinical placement in an MRI setting. Previous experience of PL was desirable but not necessary. Strategic sampling was chosen to obtain a diverse sample.[13] A total of 12 students agreed to take part in an interview. Characteristics of the students were collected (see Table 1), 11 students had experience of PL, of whom three had experience of PL in an MRI setting.
| Female | 8 |
| Male | 4 |
| 21-30 | 8 |
| ≥ 31 | 4 |
| 5th semester | 7 |
| 6th semester | 1 |
| Recently graduated | 4 |
| No | 1 |
| Yes | 11 |
| No | 9 |
| Yes | 3 |
Preceptors at seven different hospitals were invited to participate in the study and 14 agreed to an interview. The inclusion criteria were registered radiographers with at least one year of work experience as radiographers who had supervised students for one supervision period in an MRI setting. Strategic sampling was chosen to obtain variety in terms of age (M=44), gender (female n=8, male n=6) and number of years in clinical practice (M=14 years, range 4-32 years), see Table 2. There were eight preceptors who had experience of supervising in accordance with PL in settings other than MRI, while four had such experience in relation to MRI.
| Variable | Frequency (n = 12) |
|---|---|
| Female | 8 |
| Male | 6 |
| 21-30 | 4 |
| 31-40 | 2 |
| 41-50 | 2 |
| 51-60 | 5 |
| ≥ 61 | 1 |
| 0-10 | 6 |
| 11-20 | 4 |
| 21-30 | 3 |
| 31-40 | 1 |
| 0-5 | 7 |
| 6-10 | 6 |
| 11-15 | 1 |
| No | 6 |
| Yes | 8 |
| No | 10 |
| Yes | 4 |
2.4Data collection
An interview guide, created by the authors, with semistructured questions was used, focusing on the strengths and challenges associated with PL. The questions in the interview guide were pilot tested. The first author performed individual interviews with three participants, one student, one preceptor and one employee with a master’s degree. Based on feedback, one additional question was added to the interview guide.
In total, sixteen interviews were performed with 26 participants, including both focus group and individual interviews. Of these, the preceptors took part in four individual interviews and five focus group interviews with two participants in each, while the students took part in five individual interviews and two focus group interviews with two and five participants, respectively. The interviews were recorded, and notes made by the first author. The interviews for the preceptors ranged from 32 to 53 minutes (M=42 minutes) and for the students from 27 to 61 minutes (M=47 minutes).
2.5Data analysis
The data analysis was conducted with qualitative content analysis inspired by Lundman and Graneheim.[15] Each interview was transcribed, resulting in 199 pages of data. The interviews were ensured having full coverage from the interview guide. A general rule was to continue interviews until data saturation was reached i.e. which occurs when categories and sub-categories in the data become repetitive, such as no new information can be gathered by further data collection.[13]
All authors read through the transcribed data material to gain a holistic perspective. The authors avoided using preconceived categories and allowed them to emerge from the data. The analysis continued in different steps: identification of meaning units and condensed meaning units with descriptions close to the text, interpretation of the underlying meaning and finally formulation of sub-categories and categories. The material resulted in 22 sub-categories, which formed four categories and one overarching theme. Throughout the analysis, the authors discussed the coding process until consensus was achieved.
2.6Ethical considerations
According to Swedish law[16] no ethical approval was required for this study. Before the interviews, the participants were informed about the study both verbally and in writing. They were told that participation in the study was voluntary and that they could withdraw at any time without consequences. Written consent was obtained before the interviews started. After each interview, the data were transcribed verbatim and anonymized to prevent identification by giving each interview participant a code in accordance with the European General Data Protection Regulation.[17] All data were handled confidentially and only available to the authors.
2.7Methodological considerations
According to Lincoln and Guba,[18] to ensure the trustworthiness of a qualitative study there are four main concepts: credibility, dependability, transferability and confirmability. Strategic sampling was chosen to obtain a diverse sample in terms of gender and age. According to Polit and Beck,[13] diversity in a sample is preferable, which was achieved in the present study (see Table 1). The interviews were conducted by the first author over a six-month period. Regardless of when the interviews were conducted, the reflections from the participants were consistent. Therefore, no discrepancy in data collection over time was identified. The analysis was conducted in close contact with the second author until consensus was achieved. The results could be transferred to other radiology departments and different settings in other regions of Sweden. It is not possible to make any assumptions concerning what impact previous experience as a preceptor has on the perception of PL.
3.Results
The data analysis resulted in one overarching theme, four categories and 22 sub-categories of students' and preceptors' description of strengths and challenges associated with PL in an MRI-setting (see Figures 1 and 2). The overarching theme Preceptorship in PL requires support and guidance from the radiology department demonstrates that in order to supervise and be supervised in accordance with PL, the preceptors need to feel that they have the support of their co-workers, employer and clinical teachers.
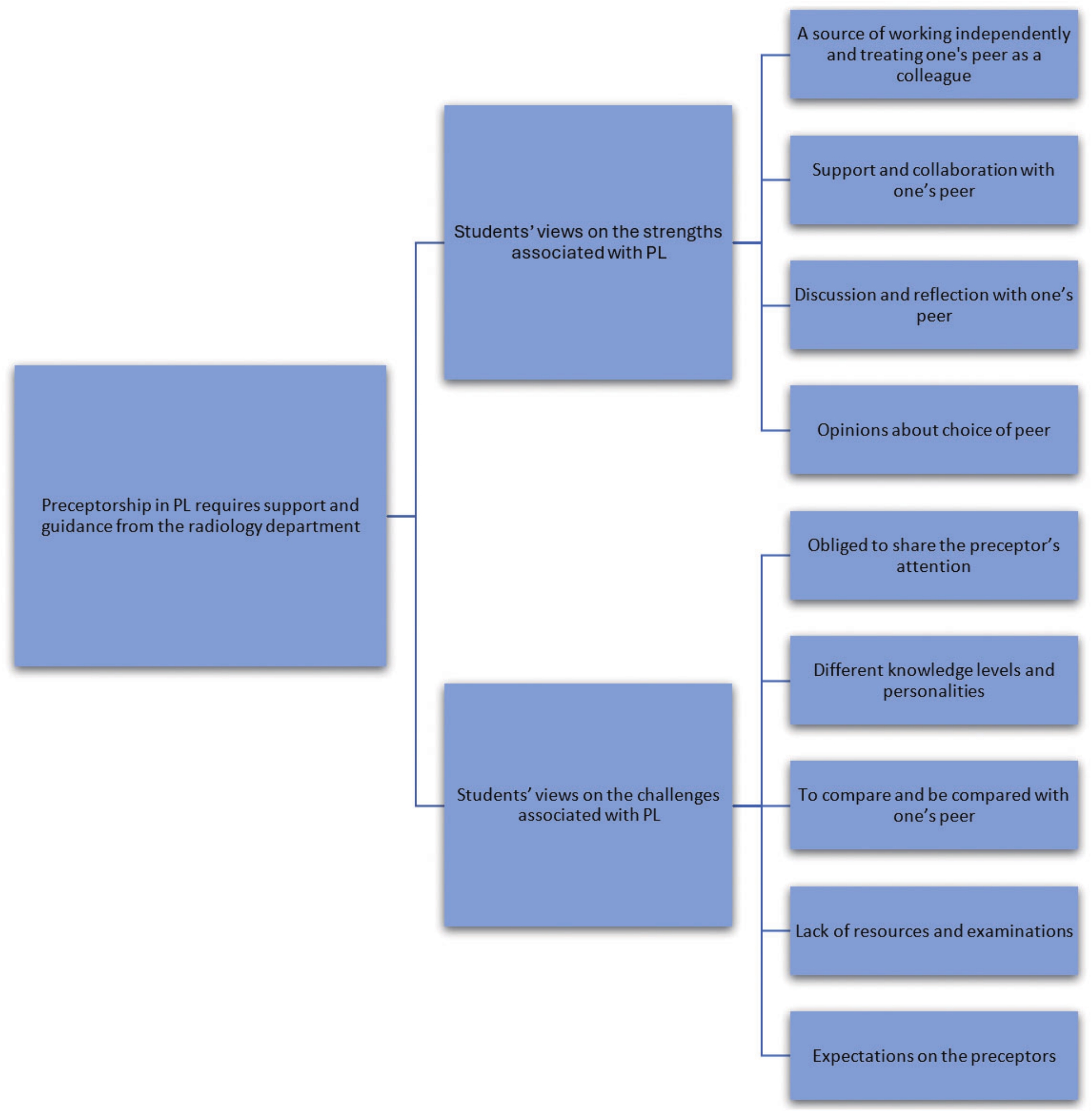
Figure 1.
Coding scheme for students with theme, categories and sub-categories
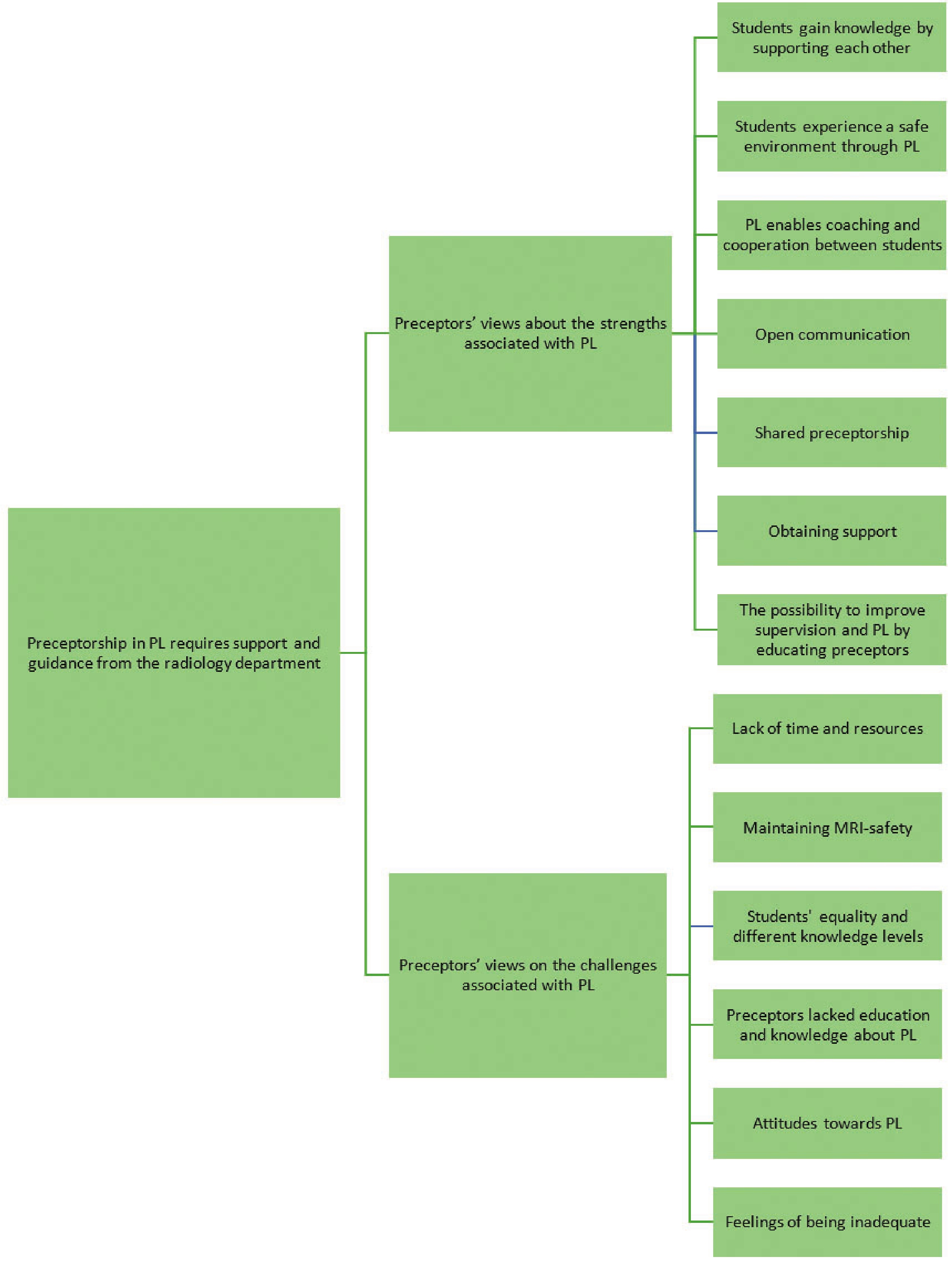
Figure 2.
Coding scheme for preceptors with theme, categories and sub-categories
3.1Students' views on the strengths associated with Peer Learning
PL can be a source of working independently and treating one’s peer as a colleague, where discussing issues with a colleague rather than a classmate increases their confidence. The students preferred the preceptor to take a step back when they were in their final year in order to rely on and pose questions to their peers instead of the preceptor.
Students described that support and collaboration with one’s peer was a strength of PL. Having a peer had a positive impact, they felt supported or supportive. The students felt more anxious and worried before their clinical placement if they were supervised alone and not according to PL. They lacked support when they had no peer to lean on.
Another strength associated with PL was discussion and reflection with one’s peer. Listening to the information several times could enhance learning. PL could also be a way to reflect on and discuss each other’s mistakes and faults. The students found it easier to discuss information with someone who was on the same level as themselves rather than the preceptor.
The students had opinions about choice of peer and believed that PL could work well if they were matched with a peer who had the same level of knowledge and a similar personality. They proposed that the university should pair students after assessing their knowledge level. However, some students also stated that they were positively surprised by their pairing and discovered that they complemented each other and worked well together despite preconceived ideas.
3.2Students' views on the challenges associated with Peer Learning
Some students experienced being obliged to share the preceptor’s attention as challenging. They stated that being alone in the MRI setting was positive, because it gave them more time to reflect. They could focus on how to perform the MRI examinations rather than observing their peer. The students indicated that being alone allowed them to learn and develop at their own pace.
Having different knowledge levels and personalities could be challenging. Some students experienced that the preceptors gave their peer more attention if they had more knowledge and were more forward and outgoing, giving them the impression of being in the background. However, some experienced it the other way around, that the preceptor gave more attention to the student who lacked knowledge. They felt obliged to step back and allow the other student to receive more attention and perform more tasks.
To compare and be compared with one’s peer was considered stressful. Some experienced that the preceptor compared them with their peer although they had different knowledge levels, which they perceived as unfair and negatively affected their confidence.
The students were concerned about the lack of resources and examinations. If there were few basic examinations that the students could perform alone at the start of their clinical placement, they expressed a concern about having to share the attention of the preceptor with peers, which limited their ability to obtain the right level of knowledge. The students mentioned that because there were too few preceptors at some hospitals, they had to be supervised in accordance with PL.
The students expressed expectations on the preceptors, such as that the preceptor needed to be prepared to supervise and communicate openly. The students suggested writing a letter to the preceptor in which they introduced themselves, adding that it was important for the preceptor to read it. They also wanted preceptors to invite them to an open dialogue about how they wanted to work and to make a plan based on that information. In addition, the students felt that it might be better to have two preceptors, as they could then give a joint opinion on the students' MRI performance and support each other.
3.3Preceptors' views about the strengths associated with Peer Learning
The preceptors stated that students gain knowledge by supporting each other. Taking a step back as a preceptor and giving students space was a good way for them to gain new knowledge and reflect together. They experienced that students increased their self-confidence when they were given more space and freedom to solve tasks together. Some preceptors believed that the MRI setting provided good conditions for PL as it was unfamiliar to both students.
Preceptors who had experience of PL as students believed that learning together and being able to supervise each other when performing various tasks was a good way of learning. The preceptors expressed that it can be easier for students to solve tasks together with someone on the same level.
The students experience a safe environment through PL, which can lead to improved performance. Having a peer could provide support, confidence and reduce feelings of isolation.
Additionally, preceptors indicated that PL could help some students who were a bit reserved. Some could find it easier to be more outgoing and discuss with and put questions to a fellow student.
Another strength preceptors discussed was that PL enables coaching and cooperation between students. The preceptors understood that PL could be challenging, especially if there were different personalities, but pointed out that it was important to learn how to adapt and work with different people. The preceptors outlined the benefits of PL, such as students having to both work together and lead each other, no one being subordinate as well as being independent of the supervisor. For instance, one student could take care of the patient, while the other could perform the MRI-examination, allowing a good division of the workload.
The preceptors thought that open communication is important, both between the students and between the student and preceptor. One of the strengths of PL is that students dare to ask each other more questions as well as put more questions to the preceptor because they can do so together.
A prerequisite for being able to supervise according to PL was shared preceptorship. This allowed preceptors to get an occasional day off from supervising. Preceptors indicated that PL was quite a demanding supervision model, thus they thought that having two preceptors made it easier to identify the students' individual needs and where they were in their learning process to enable reflection and discussion.
The preceptors considered that obtaining support was important. If they felt supported, they were more confident. They suggested this was especially an advantage if there was a problem with one student because they needed support and guidance to deal with the situation.
The preceptors stated that it was important for management to listen to their needs and fulfil them as well as valuing the work they did as preceptors.
The possibility to improve supervision and PL by educating preceptors was considered another strength. The preceptors were eager to learn more and obtain further education about PL. One preceptor who had supervision and PL education mentioned that there were several advantages in gaining increased PL knowledge, because it could help preceptors identify where the students were in their learning process.
The preceptors described that there was a need for PL education. They suggested that it could take the form of a short lecture at the radiology department or a lecture online. They also mentioned that it would be good to be able to meet other preceptors and discuss how to supervise and exchange experiences and knowledge.
3.4Preceptors' views on the challenges associated with Peer Learning
Lack of time and resources was a concern. It was stated that there is a need for more preceptors with competence in MRI to be able to keep an eye on both students and not become overwhelmed.
The preceptors discussed that having to work evening and weekend shifts and therefore not always be available to supervise students was challenging. They described that sometimes students could have up to three different preceptors instead of the main preceptor, which made it difficult for them to know what the student had learned or if they had not had the opportunity to learn something new.
Maintaining MRI-safety was another challenge. The preceptors expressed that it could be problematic to keep an eye on two students to prevent mistakes happening.
They mentioned that it was important to continuously remind the students about MRI-safety, but it could feel frightening to let the students work together without a preceptor present in the MRI room. It could be overwhelming for one preceptor with two students trying to manage everything with the patient, MRI safety and the examination.
Students' equality and different knowledge levels could be challenging. Some of the preceptors had experience of PL as students and described both strengths and challenges. Having different personalities and not being equal led to conflict and competition between students and peers. Furthermore, they reported that if the students were too similar and both were dominant, it could also lead to competition, which could be difficult to handle. Another problematic situation was if the students had different levels of knowledge, which could lead to either the students supporting and complementing each other or hiding behind each other.
Some preceptors expressed that PL was better in higher semesters and not during the first year of education because, students should find their role and learning style before working together in pairs.
Many of the preceptors lacked education and knowledge about PL and experienced that they had not been properly informed about it. They expressed concern about having to supervise according to PL one day and not knowing how to set up the supervision period. Better education in supervision and PL could contribute to colleagues viewing PL more favourably and boost their confidence.
Supervision education was a good way to develop their preceptor role. This could be an important way to remain stimulated and continue to develop in their work role. Being well prepared meant that they could create better conditions for students and more easily identify where they were in their learning process.
During the interviews different attitudes towards PL emerged. One of the preceptors who had experience of PL, both as a student and as a preceptor in an MRI setting, talked about how some of the preceptors did not agree with how to supervise in accordance with PL. These preceptors were reluctant to try PL due to having negative preconceptions about it. Some preceptors also experienced that colleagues who were not involved in preceptorship had negative attitudes towards PL, as they expressed that having two students in the MRI setting was annoying.
The preceptors expressed feelings of being inadequate and experienced that PL put high demands on them by having to divide their attention between the students. They discussed that having two students required more from the preceptor and that it was easier to be able to focus on one student. The need to adapt the supervision to both students is something that the preceptors expressed concern and felt stressed about. The preceptors experienced that PL is more time consuming than other supervision models and that managing two students in addition to their everyday work was often too much.
4.Discussion
According to both preceptors and students, the greatest strengths of PL were the feeling of safety as well as being able to work as colleagues and support each other. The preceptors reported that the students felt safe and relaxed, which enabled them to perform better and be supported throughout the learning process. PL can have positive outcomes, such as students becoming more independent and gaining confidence. Therefore, supervision in accordance with PL could be of significant value. Other studies have reported the same benefits.[19, 20, 21, 22]
During the interviews the preceptors pointed out that they lacked formal supervision education as well as education in PL. The students mentioned that they noticed if preceptors were interested in supervising and that those who were knowledgeable about PL were more confident. In contrast, lacking education and not being well informed about PL could contribute to the negative attitude towards PL on the part of some preceptors and colleagues. Preceptors also described feeling inadequate because PL was very time consuming and the need to supervise two students placed high demands on them. A study by Jassim et al.[23] reported the same challenges with PL and argued for more managerial support and for extra time to be allocated for supervision. A study by Hall-Lord et al.[1] revealed that preceptors had many years of experience in the profession but often lacked academic and pedagogy training.
Gholizadeh et al.[24] suggest that clinical teachers have an important role in supporting the preceptors, as they can guide the preceptors and provide education. However, the above authors reported that the preceptors described the same issues with low levels of perceived support from their co-workers and department. Having a supportive environment and coworkers could contribute to a better experience for the preceptors. Other studies have also shown that preceptors wished for more education to improve their teaching.[22, 25] One way to address this issue could be that all radiographers on the ward receive some education about PL, even if they do not directly supervise students. Having everyone well informed about PL could create better conditions for the preceptors to supervise students and make them feel supported. During the interviews the preceptors expressed that education could contribute to feelings of being stimulated in their profession and help them to further develop. They suggested that a lecture about supervision and PL, as well as meeting other preceptors to discuss and exchange experiences, could be helpful. This is in line with what other studies have suggested as beneficial for the preceptor role.[24, 25]
The preceptors experienced PL as time consuming and expressed a concern about the lack of staff. Mamhidir et al.[4] argued that supervising two students at a time is not more time consuming than supervising one. Implementing PL with management support can contribute to making the supervision of two students less time consuming and create good preconditions for PL. Two preceptors working together who can support each other was something that the preceptors were positive about. Sharing responsibility and work would have a positive effect because the preceptors could help each other, hence students would probably not have to be supervised by many different preceptors. Vuckovic and Landgren[26] reported the same benefits with two preceptors and recommended alternating the one responsible for two students. Another challenge mentioned by the preceptors and students was that it could be problematic if the students had different knowledge levels and personalities, which could lead to conflict and competition. It is recommended that prior to clinical placements, strategies are implemented to address conflicts in case such issues arise.[27] According to Stenberg and Carlson,[8] competition can be positive, especially for students in the final year of education. As competition can be motivating and make people perform better when comparing themselves with their peers, it can be a positive experience. Competition can also result in students identifying their personal learning needs and taking action to achieve their intended learning outcomes. If strategies were implemented to deal with conflicts and competition between students, it would give preceptors more knowledge of how to better deal with such issues, transforming them into something positive for the students.
There are trends in the data indicating that recently graduated preceptors with previous experience of being supervised in accordance with PL have a more positive perspective. This is an implication for future research.
Limitations
The small sample of 14 preceptors and 12 students limited the generalizability of the findings. A total of 11 out of the 12 students and eight of the 14 preceptors had previous experience of PL in other settings. Even though only three students and four preceptors had such experience in association with MRI, rich data about PL in an MRI setting, positive as well as negative, could be extracted from the interview transcripts. Due to scheduling conflicts, there was only one focus group interview that consisted of five participants, while the other six consisted of just two participants, which could be seen as a weakness. However, despite only one focus group having more than four participants, a great deal of material could be extracted.
5.Conclusion
Implementing PL in the clinical placement in an MRI setting requires PL education for both students and preceptors as well as support and guidance from the universities and radiology departments involved. The results reveal that students and preceptors have similar views on the challenges and strengths of PL, both groups requiring education in supervision and specifically in PL. Otherwise there is a risk that the students' learning process will be negatively impacted. The preceptors required deeper knowledge of PL, but all radiographers at the radiology department also needed to be educated about PL in order to support their preceptor colleagues. Therefore, it is important that everyone is well informed about the preceptorship model. The results of this study could be taken into consideration when implementing PL in an MRI setting.
Authors contributions
The authors have agreed on the final version of the manuscript. They have made substantial contributions to the study’s design, the acquisition, interpretation or analysis of data. The first author, Anna Palm, was primarily responsible for drafting the manuscript, performing the interviews and analysed the data. Both authors were actively involved in revising the work critically for important intellectual content. Furthermore, the authors agreed to be accountable for all aspects of the work and declared that the opinions expressed are their own.
Funding
The linguistic revision was funded by the Department of Health Sciences, Lund University, Sweden.
Conflicts of Interest Disclosure
The authors declare that they have no known competing financial interests or personal relationships that could have appeared to influence the work reported in this paper.
Informed consent
Obtained.
Ethics approval
The Publication Ethics Committee of the Association for Health Sciences and Education. The journal’s policies adhere to the Core Practices established by the Committee on Publication Ethics (COPE).
Provenance and peer review
Not commissioned; externally double-blind peer reviewed.
Data availability statement
The data that support the findings of this study are available on request from the corresponding author. The data are not publicly available due to privacy or ethical restrictions.
Data sharing statement
No additional data are available.
Acknowledgements
We greatly appreciate the valuable contributions from the medical imaging departments in southern Sweden; the preceptors, the third-year students in the radiography program, and all team members who assisted in conducting the study and generously took the time to participate.
References
- Hall-Lord M, Theander K, Athlin E. A clinical model in bachelor nursing education-Purpose, content and evaluation. Nurse Educ Pract. 2013;13(6):505-11. PMID:23465848 doi:10.1016/j.nepr.2013.02.006
- Budgen C, Gamroth L. An overview of practice education models. Nurse Educ Today. 2008;28(3):273-83. PMID:17629596 doi:10.1016/j.nedt.2007.05.005
- Andrews G, Brodie D, Andrews J. Professional roles and communications in clinical placements: A qualitative study of nursing students’ perceptions and some models for practice. Int J Nurs Stud. 2006;43(7):861-74. PMID:16380124 doi:10.1016/j.ijnurstu.2005.11.008
- Mamhidir A, Kristofferson M, Hellström-Hyson E. Nursing preceptors’ experience of two clinical education models. Nurse Educ Pract. 2014;14(4):427-33. PMID:24512652 doi:10.1016/j.nepr.2014.01.010
- Zwedberg S, Alnervik M, Barimai M. Student midwives perception of peer learning during their clinical practice in an obsteric unit: A qualitative study. Nurse Educ Today. 2021;99:104785. PMID:33524896 doi:10.1016/j.nedt.2021.104785
- Tveiten, S. Yrkesmässig handledning. Lund; Studentlitteratur. 2010.
- Boud D, Cohen R, Sampson J. Peer Learning in Higher Education: Learning from and with Each Other. London; Routledge. 2014.
- Stenberg M, Carlson E. Swedish student nurses’ perception of peer learning as an educational model during clinical practice in a hospital setting–an evaluation study. BMC Nursing. 2015;14:48. PMID:26435698 doi:10.1186/s12912-015-0098-2
- Hellström-Hyson E, Mårtensson G, Kristofferzon M. To take responsibility or to be an onlooker. Nursing student’s experience of two models of supervision. Nurse Educ Today. 2012;32(1):105-10. PMID:21388721 doi:10.1016/j.nedt.2011.02.005
- Pålsson Y, Mårtsson G, Swenne C. A peer learning intervention for nursing students in clinical practice education: A quasi-experimental study. Nurse Educ Today. 2017;51:81-7. PMID:28142097 doi:10.1016/j.nedt.2017.01.011
- Statistics Sweden. Trender och Prognoser 2020 [Internet]. Solna; Statistics Sweden. 2021. https://www.scb.se/contentassets/3fbf2376d5aa43d6a8c52b7911bd3f59/uf0515_2020i35_br_am85br2101.pd
- Lund University. VGRRS, Röntgensjuksköterskepgrogrammet, 180 högskolepoäng [Internet]. Lund; Lund University, Medicinska fakulteten. 2021. https://www.lu.se/lubas/i-uoh-lu-VGRRS
- Polit D, Beck C. Nursing Research: Generating and Assessing Evidence for Nursing Practice. Wolters Kluwer HealthPhiladelphia. 2020.
- Pickup L, Nugent B, Bowie P. A preliminary ergonomic analysis of the MRI work system environment: Implications and recommendations for safety and design. Radiography. 2019;25(4):339-45. PMID:31582242 doi:10.1016/j.radi.2019.04.001
- Graneheim U, Lundman G. Qualitative content analysis in nursing research: concepts, procedures and measusres to achieve trustworthiness. Nurse Educ Today. 2004;24(2):105-12. PMID:14769454 doi:10.1016/j.nedt.2003.10.001
- Sweden Act concerning the Ethical Review of Research Involving Humans. SFS 2003:460 [Internet]. Stockholm; Swedish Ethical Review Authority. 2003. https://www.riksdagen.se/sv/dokument-och-lagar/dokument/svensk-forfattningssamling/lag-2003460-om-etikprovning-av-forskning-som_sfs-2003-460/
- European Union Agency for Fundamental Rights. The General Data Protection Regulation: one year on: civil society: awareness, opportunities and challenges. Publications Office. 2019. https://data.europa.eu/doi/10.2811/538633
- Lincoln Y, Guba E. Naturalistic inquiry: Beverly Hills. California; SAGE Publ Inc. 1985. doi:10.1016/0147-1767(85)90062-8
- Putri S, Sumartini S. Integrating Peer Learning Activities and Problem-Based-Learning in Clinical Nursing Education. SAGE Open Nurs. 2021;7:23779608211000262. PMID:33912670 doi:10.1177/23779608211000262
- Markowski M, Bower H, Essex R. Peer learning and collaborative placement models in health care: a systemativ review and qualitative synthesis of the literature. J Clin Nurs. 2021;30(11-12):1519-1541. PMID:33461240 doi:10.1111/jocn.15661
- Vuckovic V, Karlsson K, Sunnqvist C. Preceptors’ and nursing students’ experiences of peer learning in a psychiatric context: A qualitative study. Nurse Educ Pract. 2019;41:102627. PMID:31751904 doi:10.1016/j.nepr.2019.102627
- Nygren F, Carlson E. Preceptors’ conceptions of a peer learning model: A phenomenographic study. Nurse Educ Today. 2017;49:12-16. PMID:27865125 doi:10.1016/j.nedt.2016.10.015
- Jassim T, Carlsson E, Bengtsson M. Preceptors’ and nursing students’ experience of using peer learning in primary healthcare settings: a qualitative study. BMC Nurs. 2022;21:66. PMID:35313874 doi:10.1186/s12912-022-00844-y
- Gholizadeh L, Shahla S, Valizadeh S. Nurse preceptors’ perceptions of benefits, rewards, support and commitment to the preceptors role in an new preceptorship program. BMC Med Educ. 2022;22:472. PMID:35715778 doi:10.1186/s12909-022-03534-0
- Bengtsson M, Carlsson E. Knowledge and skills needed to improve as preceptor: development of a continuous professional development course – a qualitative study part I. BMC Nursing. 2015;14:51. PMID:26478717 doi:10.1186/s12912-015-0103-9
- Vuckovic V, Landgren K. Peer learning in clinical placements in psychiatry for undergraduate nursing students: preceptors and students’ perspective. Nurs open. 2021;8(1):54-62. PMID:33318812 doi:10.1002/nop2.602
- Secomb J. A systemativ review of peer teaching and learning in clinical education. J Clin Nurs. 2008;17(6):703-716. PMID:18047577 doi:10.1111/j.1365-2702.2007.01954.x


